Well we had a very good meeting with Endocrine today. It was the best meeting we've had with Endocrine. We had quite a few areas of discussion today. Our next appointment will be in 4 months instead of 6 months.
Beginning with Haven's blood pressure being slightly on the rise and today at the doctor her blood pressure was 125/67 and a heart rate of 125. Which the heart rate I'm used to but I noticed last night her blood pressure was 124/63. Which is pretty high. We discussed with Endo and it's possible that her blood pressure medication may need to be reevaluated and increased. We will discuss with Oncology on our next visit. Cyclosporin can also raise the blood pressure.
Next up was Haven's growth. While I have been happy that between January and April she has grown from 39 1/2 inches to 41 1/2 inches it seems as though this is not enough. Haven is around the 5th percentile for height. We had a pretty long discussion as I really do not want to have to put her on growth hormone shots. Our friend Josh is on them and I believe he gets 6 shots a week....I think Haven would beat me up if I tried to do that! :) The doctor said he would not put her on this yet but he said he had to see her grow a lot more in the next 4 months than she has in the last 6 months. If she does not grow a lot over the next 4 months she will have her IGF1 retested and probably begin the shots. Haven's current IGF1 level is 55 and normal is between 57 - 260.
Haven has her Thyroid checked about every few months and as of right now she is looking good. Actually I had to have some blood work done last week and her Thyroid is better than mine! So this is great news. Kris has been concerned with Haven's sodium levels - which over the past 3 months of lab work she has remained in the healthy zone - not high like she was before we started back on chemo.
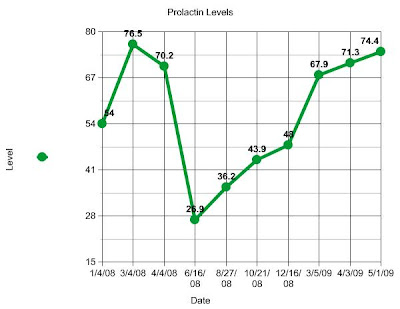
The above chart is something I made with the info received today about Haven's Prolactin level. In the early months of 2008 we didn't really monitor this very close. In October I began a lot of research and was extremely concerned about the Prolactin level. The doctors weren't really monitoring it because nothing has ever really been noted about Prolactin in ROHHAD children. I was very emotional about checking this constantly that the doctors have now started to look closely at it. The graph above shows the dates Haven's Prolactin was checked and the level it was at. This shows us that the Hypothalamus is not communicating with the Pituitary.
We discussed the time in the graph where Haven was at her lowest on Prolactin level. This was the best Haven has ever been in 3 years. She completely stopped wearing diapers, she was refusing food and never asked for it, she was sleeping soundly, never sleep walking or talking, behavior was awesome. This was when Haven was on Rituximab and Cytoxan. So as I have been questioning over the past few weeks in my head with the minimal progress we've made on Rituximab. Was it the Rituximab? Was it the Cytoxan? Was it the combination of both at the same time? I believe this is a hint to what we will find out in 4 more months from Oncology. I won't make a guess here but I have a pretty good feeling I'm right.
Cortisol - Cushing's testing -- We discussed retesting Haven for Cushing's Syndrome with the salivary test. Her last Cortisol reading was done in January when she was taken of Prednisone and it was at a good level. The doctor pretty much left this decision up to me and what I wanted to do. I talked to Kris and then told the doctor that I felt I would like to wait until our meeting in 4 months to do the test. High cortisol will stop you from growing. Since Haven has grown this may be more that she doesn't need to deal with right now. He agreed. So in 4 months if Haven has not grown almost twice as much as she has in the past few months we will test the Cortisol.
At most our Endo doctor will only do the salivary testing for Cushing's. If we find that her levels are not normal he will refer us to a doctor at NIH for further testing. He is not familiar with all the types of Cushing's and the doctors down there specialize in this. Knowing Susannah also went to NIH makes me feel more comfortable with going there to be tested. The reason we can not do the pee test on Haven is because she is still in full-time diapers. She would have to be admitted to the hospital for a week on a catheter to get all of her urine. I do not want her to have to do this if it's not necessary. So in September we will move forward with this.
I feel really great about our meeting and the decisions we've come to together. Kris said he felt very comfortable with it all. We continue with our current list of medications, checking her blood pressure twice a day, and monitoring her on the pulse ox machine at night.
Thank you to everyone for all your help.
If Haven does have to have growth hormone shots, make sure and let her know that they do not hurt. The needle is teeny tiny and is a very little poke - much less than any bloodwork she's had to have or anything like that. Josh has not once complained with the shots. He likes to take them in the back of his arms. He wants the shots because he likes growing taller. :)
ReplyDeleteI'm glad your Endocrinology visit was so successful!
It's great that you left the doctor feeling good about the decisions you have made. As parents, sometimes when we leave we feel pretty horrible. :S
ReplyDeleteMake sure you check out the Tuesday F. Whitt Annual blog party auction, and help researchers find a cure for neuroblastoma, one of the least funded pediatric cancers, and one of the most deadly at http://www.fundraiserblog.blogspot.com/